Dr. Silver explained that HIFU destroys only the diseased part of the prostate, which means that side effects like urinary incontinence and not being able to have sex are less likely. This is unlike radical surgery or radiation which both are riskier for these 2 side effects. Also HIFU is done quickly (approximately two to three hours), in a single session and at an outpatient surgery center, away from the main hospital, so I could get in and out quickly, and avoid any risk of contracting Covid.
Author: Paulo Martins
Podcast: Focal One therapy HIFU
Christopher Weight, MD, Center Director of Urologic Oncology at Cleveland Clinic joins the Cancer Advances podcast to discuss how high-intensity focused ultrasound (HIFU), a type of focal therapy for treating localized prostate cancer, is emerging as an alternative to more traditional treatments, such as surgery and radiation for select patients.
New Orleans Music Producer Shane Norris Diagnosed with Prostate Cancer During Covid Shares His Journey with HIFU Treatment
Shane shares the experience he had navigating the Covid pandemic as he searched for the prostate cancer treatment that he felt best suited his needs. With financial support raised from a GO-Fund-Me project as well as help and guidance from a number of resources, including medical professionals, family and friends, Shane decided to become the first man in Louisiana to treat his prostate cancer with high intensity focused ultrasound – or HIFU.
Dad on Road to Recovery after Ultrasound Therapy for Prostate Cancer
An Ohio father is opening up about his battle with prostate cancer — the most common cancer among men in the u-s after skin cancer. He never thought it could happen to him but thanks to a non-invasive therapy using sound energy, he’s back in the driver’s seat.
Focal One® High-Intensity Focused Ultrasound
To learn more about prostate cancer treatment options, please visit Cleveland Clinic website.
An update on prostate cancer treatment [PODCAST]
“Even though prostate cancer patients are anxious to receive treatment, they still want to minimize their exposure to anyone outside their COVID bubble. One procedure that is especially attractive to our patients is focal therapy high intensity focused ultrasound (HIFU).
Focal therapy HIFU is appropriate for patients whose prostate cancer is diagnosed at a higher grade and stage, but is still confined to the prostate. We use guided imagery to locate and destroy only the diseased portion of the prostate. It is done quickly (approximately two to three hours), in a single session. Patients like the ability to get in and out, with minimal exposure to the health care system. Focal therapy HIFU is ideal for this.”
Man Benefits from Focused Ultrasound Therapy for Prostate Cancer
HIFU is high-intensity focused ultrasound, an innovative prostate cancer treatment that uses the energy of sound waves to pinpoint, heat and kill prostate cancer cells. Unlike forms of radiation and surgery, HIFU is a noninvasive outpatient procedure that leaves healthy tissue unharmed.
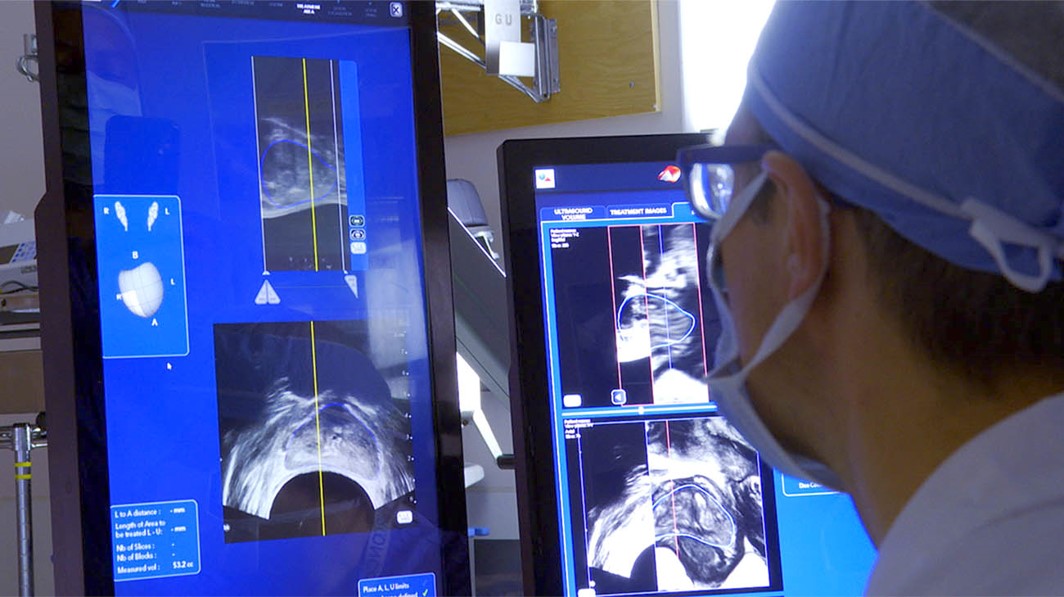
New technology leads to more accurate prostate cancer diagnosis and treatments
If the disease has spread to the bones or elsewhere outside the prostate, targeted therapies such as hormonal treatment, chemotherapy, radiopharmaceuticals, immunotherapy and focused radiation can be employed.
Parekh and his Sylvester team use high-intensity focused ultra-sound, or HIFU, which fuses MRI and biopsy data with real-time ultrasound imaging that allows urologists to view detailed 3D images of the prostate.
Read more here: https://www.miamiherald.com/living/health-fitness/article251288899.html#storylink=cpy



![An update on prostate cancer treatment [PODCAST]](https://us.hifu-prostate.com/wp-content/uploads/2021/06/podcast-kevinMD.jpg)